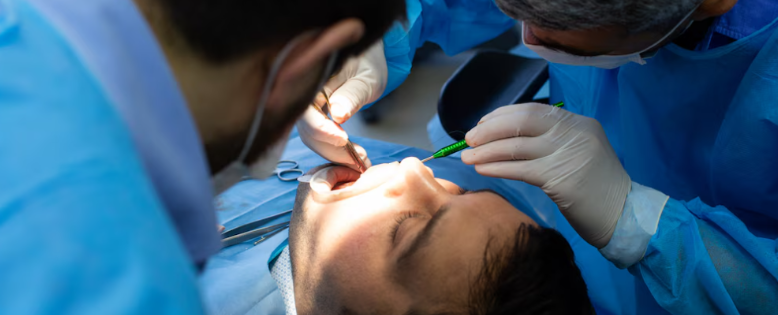
Oral surgery in Finchley N12 refers to a range of surgical procedures performed within the mouth and jaw to treat conditions that cannot be resolved through routine non-surgical dental treatment. From tooth extractions and wisdom tooth removal to dental implant placement, cyst removal, and corrective jaw procedures, oral surgery addresses some of the most complex and significant dental health concerns that patients encounter throughout their lives. If you have been referred for oral surgery or are experiencing symptoms that suggest a surgical solution may be necessary, finding a trusted Dental Clinic in Totteridge with the clinical expertise and patient-centered approach to guide you safely through the process is the most important step you can take toward resolution and recovery.
Oral surgery can sound daunting to patients who have not experienced it before, and it is entirely natural to have questions and concerns about what the process involves, what recovery looks like, and how to ensure the best possible outcome. The reality is that modern oral surgical techniques, combined with effective local anesthesia and carefully planned aftercare, make the vast majority of oral surgical procedures far more manageable and comfortable than most patients anticipate. For residents seeking comprehensive Dental Care in Totteridge that includes the full range of surgical dental treatments, having a knowledgeable and compassionate dental team to support you at every stage of your care makes the entire experience significantly less stressful and more straightforward.
What Is Oral Surgery
Oral surgery is the branch of dentistry concerned with the diagnosis and surgical treatment of diseases, injuries, and defects affecting the teeth, gums, jawbone, and other structures of the mouth and face. It encompasses both minor surgical procedures that are routinely performed in a dental practice under local anesthesia and more complex procedures that may require referral to a hospital or specialist oral and maxillofacial surgeon.
The goal of oral surgery is always to restore health, function, and comfort to the patient by addressing conditions that have progressed beyond the reach of non-surgical dental treatment. In many cases, timely oral surgery prevents more serious complications, preserves surrounding structures, and provides a foundation for further restorative or cosmetic dental work that improves the patient’s quality of life significantly.
A skilled Dentist in Totteridge who provides oral surgical services will begin with a thorough assessment of the affected area, review your medical history carefully, and explain all available treatment options with complete transparency before any surgical procedure is recommended or undertaken.
Totteridge Dental Studio is one of the best dental clinics in Totteridge, providing a comprehensive range of oral surgical procedures to patients across Finchley N12 and the surrounding areas of North London. Located at 59 Totteridge Ln, London N20 0HD, United Kingdom, the studio combines clinical precision with a genuine commitment to patient comfort and clear communication throughout every stage of treatment. You can reach the team at info@totteridgedental.co.uk or by calling +44 20 8445 5024 to book a consultation and discuss your oral surgical needs with a qualified and experienced dental professional.
Common Types of Oral Surgery Procedures
Oral surgery covers a wide spectrum of procedures, ranging from straightforward extractions to more involved surgical interventions. Understanding the most commonly performed oral surgical procedures helps patients recognize when surgery may be necessary and what each procedure involves.
Tooth Extractions
Tooth extraction is the most commonly performed oral surgical procedure. When a tooth is so severely decayed, fractured, or damaged that it cannot be saved through any restorative means, extraction is the most appropriate clinical option. Extractions are also performed when a tooth is causing overcrowding that is compromising orthodontic treatment, when a tooth is impacted and causing pain or infection, or when a tooth is associated with a periapical abscess that cannot be resolved through root canal treatment.
Simple extractions involve the removal of a tooth that is fully erupted above the gumline and can be accessed directly with dental instruments under local anesthesia. Surgical extractions are required for teeth that are broken at the gumline, impacted below the surface of the gum, or otherwise not accessible through a simple extraction approach. Surgical extractions involve making a small incision in the gum tissue and may require the removal of a small amount of surrounding bone to access and remove the tooth in sections.
Wisdom Tooth Removal
Wisdom teeth, also known as third molars, are the last teeth to emerge and frequently cause problems due to a lack of space in the jaw to accommodate them properly. Impacted wisdom teeth are those that are unable to erupt fully or at all because they are blocked by existing teeth, bone, or soft tissue. Partially erupted or fully impacted wisdom teeth are associated with pain, infection, cyst formation, damage to adjacent teeth, and crowding of the existing dentition.
Wisdom tooth removal is one of the most frequently performed oral surgical procedures and ranges in complexity from straightforward erupted extractions to complex surgical removals of deeply impacted teeth. The procedure is performed under local anesthesia and typically involves a short recovery period during which mild swelling, soreness, and limited mouth opening are normal and expected responses to the surgical intervention.
Dental Implant Placement
Dental implant surgery involves the placement of a titanium implant fixture into the jawbone to serve as an artificial tooth root, upon which a crown, bridge, or denture is subsequently attached. Implant placement is a minor surgical procedure performed under local anesthesia that requires careful pre-surgical planning including assessment of bone volume and density, the relationship of the implant site to adjacent anatomical structures, and the patient’s overall medical health.
Following placement, the implant undergoes a process called osseointegration during which the surrounding bone fuses to the implant surface over a period of several months. Once integration is confirmed, the final restorative component is attached to complete the tooth replacement. Dental implants are widely regarded as the most functional and aesthetically natural tooth replacement option currently available in dentistry.
Surgical Removal of Cysts and Lesions
Cysts and lesions in the jaw and soft tissues of the mouth can arise from a variety of causes including infection, developmental abnormalities, and in rare cases, pathological processes that require investigation. Surgical removal of cysts involves accessing the cyst through an incision in the overlying gum or bone, carefully removing the cyst in its entirety, and sending the removed tissue for histological examination to confirm its nature. Regular dental examinations and X-rays are the most reliable way to detect cysts and lesions before they become symptomatic or cause significant bone destruction.
Bone Grafting
Bone grafting procedures are performed to restore the volume and density of jawbone that has been lost as a result of tooth extraction, gum disease, injury, or infection. Adequate bone volume is essential for the successful placement of dental implants, and bone grafting is often a necessary preparatory step for patients who have experienced significant bone loss in the implant site. Bone graft material may be taken from another site in the patient’s own body, from a donor source, or from a synthetic bone substitute, depending on the volume required and the specific clinical situation.
Frenectomy
A frenectomy is the surgical removal or modification of a frenum, which is a small fold of tissue that connects the lips or tongue to the gum or floor of the mouth. An overly tight or thick frenum can restrict tongue movement, cause a gap between the front teeth, or contribute to gum recession in the area. Frenectomy is a minor and quick surgical procedure with a straightforward recovery that can significantly improve function and aesthetics when indicated.
Signs That You May Need Oral Surgery
Recognizing the signs that suggest oral surgery may be necessary allows you to seek professional assessment promptly and avoid the complications that arise from delayed treatment. The following are among the most common indicators that a surgical evaluation is warranted.
Persistent pain in a tooth or jaw area that does not respond to non-surgical treatment or medication may indicate the presence of an impacted tooth, cyst, abscess, or other condition requiring surgical intervention. Swelling in the jaw, cheek, or gum tissue that does not resolve with antibiotics or that recurs repeatedly is a sign that the underlying cause needs to be addressed surgically.
Difficulty opening the mouth fully, restricted jaw movement, or jaw pain that affects eating and speaking may indicate a condition affecting the jaw joint or the surrounding structures that requires further investigation and potentially surgical management. A tooth that remains unerupted well beyond its expected eruption time may be impacted and may need surgical assistance to be accessed, repositioned, or removed.
Visible or palpable lumps or swellings in the soft tissues of the mouth, jaw, or neck that persist for more than two weeks without a clear and resolving cause should always be assessed by a dental professional without delay, as some oral lesions require biopsy and histological examination to confirm their nature.
Teeth that are too damaged, broken, or infected to be saved through any conservative means are candidates for surgical extraction. Significant bone loss in the jaw as a result of periodontal disease, tooth loss, or injury may indicate the need for bone grafting to restore the structural foundation of the jaw before further restorative treatment can proceed.
For patients who want to understand the full range of oral surgical options available locally, the Oral Surgery in Finchley N12 London page at Totteridge Dental Studio provides detailed information about the surgical services available and what the treatment process involves.
Step-by-Step: What to Expect During Oral Surgery
Understanding the complete process of oral surgery from the initial consultation through to recovery helps patients feel fully prepared and significantly reduces the anxiety that often surrounds surgical dental treatment.
Step 1: Consultation and Comprehensive Assessment Your oral surgery journey begins with a detailed consultation during which your dental team will take a thorough medical and dental history, examine the area requiring treatment, and take any necessary diagnostic imaging including dental X-rays or CBCT scans to assess the surgical site in detail. The clinical findings will be discussed with you clearly and all available treatment options will be explained before any recommendations are made.
Step 2: Medical History Review and Treatment Planning Before any oral surgical procedure is scheduled, your medical history will be reviewed carefully to identify any conditions or medications that may affect the surgical approach, the choice of anesthesia, or the healing process. Patients on blood thinning medications, immunosuppressants, bisphosphonates, or other medications that can affect healing will need to discuss this with their dental team and in some cases their medical practitioner before proceeding. A detailed treatment plan outlining the procedure, the anesthesia approach, the expected recovery timeline, and the aftercare requirements will be provided and discussed.
Step 3: Preparation Before the Procedure Your dental team will provide specific pre-operative instructions tailored to your procedure. These may include guidance on eating and drinking before the appointment, arrangements for transport home if sedation is being used, the temporary cessation of certain medications, and any other preparations specific to your individual situation and the nature of the surgery planned.
Step 4: Administration of Anesthesia On the day of your procedure, the area to be treated will be thoroughly numbed with local anesthesia before any surgical work begins. Your dental team will ensure that the anesthetic has taken full effect and that you are completely comfortable before proceeding. If you are particularly anxious about the procedure, conscious sedation options may be available and can be discussed with your dental team during the planning stage.
Step 5: The Surgical Procedure The surgical procedure will be carried out with precision and care, following the treatment plan established during the consultation and planning stage. Your dental team will communicate with you throughout the procedure and will check on your comfort at regular intervals. If at any point you experience discomfort, alerting your dental team immediately allows them to administer additional anesthesia before continuing.
Step 6: Immediate Post-Operative Care Once the procedure is complete, your dental team will apply any necessary dressings or sutures, provide clear verbal and written post-operative instructions, and ensure that you are stable and comfortable before you leave the clinic. You will be advised on what to expect in terms of swelling, soreness, and bleeding in the hours and days following surgery, and you will be given guidance on pain management, dietary restrictions, oral hygiene during recovery, and activity limitations.
Step 7: Recovery and Follow-Up Recovery from oral surgery varies depending on the nature and extent of the procedure. Minor procedures such as simple extractions typically involve a recovery period of a few days. More complex surgical procedures may require a longer period of healing with more significant restrictions on activity and diet. Attending your scheduled follow-up appointment allows your dental team to assess your healing progress, remove any sutures that are not self-dissolving, and address any concerns that have arisen during recovery.
Common Patient Mistakes Around Oral Surgery
Being aware of the most frequent errors that patients make before, during, and after oral surgery helps you avoid decisions that compromise the outcome of your treatment or prolong your recovery.
Not disclosing the full medical history and current medications before oral surgery is a potentially serious mistake. Certain medical conditions and medications significantly affect bleeding, healing, and the safety of anesthesia. Your dental team needs complete and accurate information to plan your surgery safely. Always inform your dental team of all medications you take, including over-the-counter products, vitamins, and herbal supplements.
Failing to arrange appropriate transport home after a surgical procedure, particularly one involving sedation, is a safety risk that should never be overlooked. Patients who have received sedation must not drive, operate machinery, or make important decisions for the remainder of the day following the procedure. Always arrange for a responsible adult to accompany you home.
Rinsing the mouth vigorously or drinking through a straw in the hours immediately following an extraction disrupts the blood clot that forms in the socket and is essential for normal healing. Dislodging this clot leads to a painful condition called dry socket that significantly delays recovery and requires additional clinical management.
Smoking following oral surgery impairs healing, increases the risk of infection, and is one of the leading causes of post-operative complications including dry socket and poor wound healing. Abstaining from smoking for at least forty-eight to seventy-two hours after surgery, and ideally for several days or longer, significantly improves the healing outcome.
Returning to strenuous physical activity too soon after oral surgery increases blood pressure and can cause renewed bleeding or disruption of the healing wound. Following the specific activity restrictions provided by your dental team for the recommended recovery period is an important part of supporting a smooth and uncomplicated healing process.
Prevention and Aftercare Tips for Oral Surgery Patients
Supporting your recovery following oral surgery and taking steps to protect your oral health going forward are both essential parts of the overall care process.
Take any prescribed medication including antibiotics and pain relief exactly as directed by your dental team. Do not stop a course of antibiotics early even if you feel better before the course is completed. Eat soft foods and avoid chewing on the surgical side of the mouth until your dental team confirms that the area has healed sufficiently to resume normal function.
Keep the surgical area clean by following the specific oral hygiene instructions provided. This typically involves gentle rinsing with a warm salt water solution from the day after surgery rather than brushing directly over the wound site immediately. Gradually resume your full oral hygiene routine as healing progresses and your dental team advises.
Attend all scheduled follow-up appointments without delay. These appointments exist to monitor your healing and address any complications at the earliest possible stage, when they are most straightforwardly managed. If you experience any unexpected symptoms such as increasing pain, significant swelling, fever, uncontrolled bleeding, or a foul taste in the mouth, contact your dental clinic promptly rather than waiting for your next scheduled appointment.
Frequently Asked Questions
- Will oral surgery be painful?
Oral surgery is performed under effective local anesthesia, which means the procedure itself should be completely pain-free. You may feel pressure and movement during the procedure but you should not feel pain at any point. After the anesthetic wears off, some degree of soreness and discomfort is normal and expected. This is typically well managed with the pain relief medications recommended or prescribed by your dental team. Most patients find that their post-operative discomfort is manageable and resolves progressively over the days following surgery.
- How long does recovery from oral surgery take?
Recovery time varies considerably depending on the type and complexity of the oral surgical procedure performed. Simple extractions typically result in a recovery period of two to five days during which soreness and mild swelling are the primary symptoms. More complex procedures such as surgical wisdom tooth removal or bone grafting may involve a recovery period of one to two weeks with more significant swelling and a longer period of dietary and activity restrictions. Your dental team will give you a realistic estimate of the expected recovery timeline for your specific procedure during the consultation and planning stage.
- Can I eat normally after oral surgery?
In the hours and days immediately following oral surgery, a soft diet is strongly recommended to avoid disturbing the surgical site and to minimize discomfort during chewing. Foods such as yogurt, soup, mashed potatoes, scrambled eggs, and smoothies are appropriate choices in the initial recovery period. As healing progresses and discomfort reduces, the diet can be gradually expanded based on your own comfort level and the guidance of your dental team. Hot, hard, crunchy, and spicy foods should be avoided until the wound has healed sufficiently.
- Do I need someone to accompany me to oral surgery?
For procedures performed under local anesthesia alone, most patients are able to travel independently to and from their oral surgery appointment. However, if your procedure involves conscious sedation, you must have a responsible adult to accompany you home and remain with you for the rest of the day as sedation temporarily impairs judgment, coordination, and reaction times. Your dental team will advise you on the specific transport and supervision requirements for your individual procedure during the planning stage.
- What should I do if I experience complications after oral surgery?
If you experience any symptoms following oral surgery that concern you, including increasing rather than decreasing pain after the first two to three days, significant swelling that is worsening rather than improving, fever, difficulty swallowing or breathing, uncontrolled bleeding, or a foul taste or odor from the surgical site, you should contact your dental clinic promptly. Do not wait until your next scheduled follow-up appointment if you are experiencing symptoms that suggest a complication. Your dental team is there to support you throughout your recovery and addressing any concerns early leads to the best possible outcomes.
Conclusion
Oral surgery in Finchley N12 covers a broad and important range of procedures that address some of the most significant dental health challenges patients face, from wisdom tooth removal and complex extractions to implant placement and cyst removal. Seeking professional assessment promptly when symptoms suggest surgery may be needed, preparing thoroughly for your procedure, and following your dental team’s aftercare guidance carefully are the three commitments that lead to the safest, most comfortable, and most successful surgical outcomes. Totteridge Dental Studio, located at 59 Totteridge Ln, London N20 0HD, United Kingdom, is one of the most trusted dental clinics in Totteridge, providing skilled and compassionate oral surgical care to patients across Finchley N12 and North London with the expertise and dedication that every patient deserves.